Dr. Vikas Singh is a highly specialized Consultant Urologist and Andrologist in Indore, offering comprehensive treatment for severe Erectile Dysfunction (ED) including advanced Penile Implant surgery. With extensive training in Andrology and reconstructive urology, he provides patients suffering from refractory ED—those who haven’t responded to medications, injections, or other conservative treatments—a definitive solution that restores spontaneous, reliable erectile function. His expertise encompasses both Inflatable Penile Prostheses (two-piece and three-piece systems) and Semi-Rigid/Malleable implants, allowing personalized device selection based on patient anatomy, lifestyle, and preferences. Practicing at Kokilaben Dhirubhai Ambani Hospital Indore with access to the latest generation prosthetic devices and specialized surgical techniques, Dr. Singh achieves high patient satisfaction rates while minimizing complications. His compassionate, discreet approach ensures comfortable discussions about this sensitive topic, comprehensive pre-operative counseling, and thorough post-operative support. We maintain complete confidentiality and transparency regarding treatment costs for our patients across Central India.
Consultant Surgeon at Kokilaben Dhirubhai Ambani Hospital, Indore, with access to latest generation penile prosthetic devices.
Advanced fellowship training in male sexual medicine and reconstructive procedures including penile prosthesis surgery.
High patient and partner satisfaction rates with restored spontaneous sexual function and improved quality of life.
Penile implants (also called penile prostheses) are medical devices surgically placed inside the penis to enable men with severe erectile dysfunction to achieve erections suitable for sexual intercourse. Unlike medications that enhance natural erections, implants provide mechanical rigidity on demand, offering a permanent solution when other treatments have failed. Modern devices are sophisticated, reliable, and designed to mimic natural erections as closely as possible.
Implants become the treatment of choice when erectile dysfunction is severe and refractory to conservative treatments—meaning oral medications (Viagra, Cialis, Levitra) are ineffective or contraindicated, intracavernosal injections fail or aren't tolerated, vacuum devices are unsatisfactory, and underlying causes (diabetes, post-prostatectomy, Peyronie's disease, pelvic trauma) make other treatments unlikely to succeed. Implants are also ideal for men seeking a permanent, reliable solution without needing to plan ahead or depend on medications.
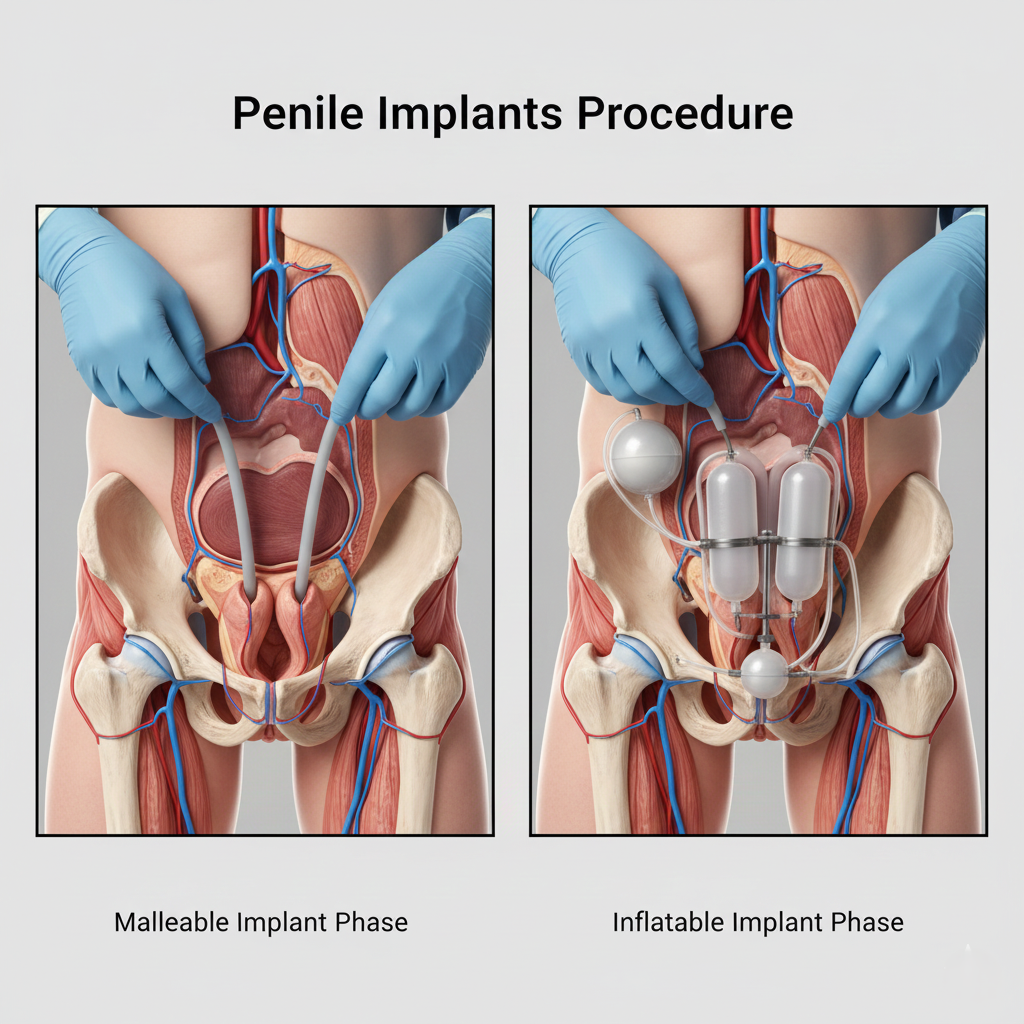
Three main categories exist: Three-Piece Inflatable Prostheses (most sophisticated, with cylinders in penis, pump in scrotum, and reservoir in abdomen—providing most natural appearance and function), Two-Piece Inflatable Prostheses (simpler system with cylinders and combined pump-reservoir—easier surgery, good functionality), and Semi-Rigid/Malleable Prostheses (bendable rods that remain firm but can be positioned—simplest design, lowest cost, ideal for patients with manual dexterity issues). Dr. Singh helps select the optimal device for each patient's specific situation.
Candidacy assessment begins with comprehensive history taking (ED duration, previous treatments tried, underlying medical conditions, relationship status), physical examination (penile anatomy, testicular examination, neurological assessment), laboratory tests (testosterone levels, diabetes screening, cardiovascular risk factors), and psychological evaluation (ensuring realistic expectations, assessing for depression or relationship issues). This thorough workup ensures patients are appropriate candidates and mentally prepared for surgery.
Dr. Singh provides detailed counseling on device options, explaining how each type functions, surgical complexity, cosmetic appearance when deflated/flaccid, ease of use, durability expectations (modern devices last 10-15+ years), potential complications, and realistic expectations about size and sensation. Patient lifestyle, manual dexterity, body habitus, and partner preferences all influence device selection. Comprehensive informed consent ensures patients understand both benefits and limitations.
Surgery is performed under spinal or general anesthesia, typically taking 60-90 minutes. Through small incisions (penoscrotal, infrapubic, or scrotal approaches), cylinders are placed inside the corpora cavernosa (erectile chambers), the pump is positioned in the scrotum for easy access, and the reservoir (for three-piece systems) is placed in the lower abdomen. Meticulous surgical technique, antibiotic-impregnated devices, and strict sterility protocols minimize infection risk—the most serious potential complication. Hospital stay is typically 1-2 days with catheter removed before discharge.
This sophisticated system most closely mimics natural erections. Squeeze the scrotal pump several times to transfer fluid from the abdominal reservoir into penile cylinders, creating rigid erection. Press the release valve to deflate, returning fluid to reservoir and allowing natural-looking flaccid state. Advantages include most natural appearance (completely concealed when deflated), best rigidity for intercourse, most natural feel for both partners, and excellent concealment under clothing. Disadvantages include more complex surgery (slightly higher complication risk), requires good manual dexterity to operate pump, and highest cost. Best for active, healthy men prioritizing natural appearance and function. Primary Advantages: Most natural erection and flaccidity, best cosmetic result, high satisfaction rates.
Simpler system with combined pump-reservoir unit in scrotum and cylinders in penis. Operation similar to three-piece but requires no abdominal reservoir, making surgery simpler and shorter. Provides good rigidity and reasonable flaccidity, though not quite as natural-looking as three-piece when deflated. Advantages include simpler surgery (lower complication risk), easier operation than three-piece, good balance of function and simplicity, and moderate cost. Best for patients wanting inflatable function but preferring simpler surgery or those with previous abdominal surgeries complicating reservoir placement. Primary Advantages: Good functionality, simpler surgery than three-piece, reasonable concealment.
Bendable rods placed in penis that remain constantly firm but can be positioned up (for intercourse) or down (for concealment). Advantages include simplest surgery (lowest complication risk), easiest to use (no pumping mechanism), most durable (fewest mechanical failures), lowest cost, and ideal for patients with limited manual dexterity. Disadvantages include always somewhat firm (less natural flaccid appearance), may be visible under tight clothing, and potential for erosion over time with constant pressure. Best for elderly patients, those with arthritis or dexterity issues, diabetics with neuropathy, or patients prioritizing simplicity and reliability. Primary Advantages: Simplest surgery and use, most reliable mechanically, lowest cost, excellent for specific populations.
Achieve erection whenever desired without planning ahead, taking pills, or waiting—spontaneous sexual activity restored.
Over 90% of patients and 70-80% of partners report satisfaction—among highest of any ED treatments.
One-time surgery provides long-term solution (devices last 10-15+ years)—no ongoing costs for medications or repeated treatments.
Penile sensation, ability to achieve orgasm, and ejaculation are preserved—only erection mechanism is replaced.
Schedule a private, confidential consultation with Dr. Singh in Indore.
Modern penile implants, especially three-piece inflatable devices, feel remarkably natural to both partners. For the man, the sensation is your own penis—skin sensitivity, ability to feel touch and pleasure, and orgasm capability remain completely unchanged since the implant is inside the erectile chambers and doesn’t affect nerve endings. When inflated, rigidity feels firm and supportive, though slightly different from natural erections (typically firmer/more uniform). For partners, most report that inflatable implants feel very natural during intercourse—the warmth, skin texture, and overall sensation are virtually indistinguishable from natural erections. The main difference partners might notice is consistent firmness regardless of duration. When deflated, three-piece implants appear quite natural in flaccid state, though experienced partners might notice slightly firmer consistency than natural flaccid penis. Semi-rigid implants are more obvious as they’re always somewhat firm. Most partners, when informed and involved in the decision-making process, are highly satisfied—studies show 70-80% partner satisfaction rates. Open communication with your partner about the implant before and after surgery significantly enhances satisfaction.
Yes—this is one of the most reassuring aspects of penile implants. The surgery involves placing devices inside the corpora cavernosa (erectile chambers) but doesn’t affect the nerves responsible for penile sensation, the ability to achieve orgasm, or the ejaculatory mechanism. Skin sensitivity remains completely intact since superficial nerves aren’t touched. The glans (head) and shaft retain full sensation to touch, temperature, and pleasure. Orgasm capability is preserved because the implant doesn’t affect the complex neurovascular pathways responsible for climax. Most men report unchanged or even enhanced orgasm quality after implants because performance anxiety is eliminated and they can focus on pleasure rather than worrying about erection loss. Ejaculation is similarly preserved since the vas deferens, seminal vesicles, and ejaculatory ducts are untouched—if you could ejaculate before surgery, you will after. The only change is the mechanism of achieving rigidity (mechanical vs. vascular). Some men report initially that orgasms feel different simply due to psychological adjustment, but this typically normalizes within 3-6 months as they become comfortable with the device.
Penile implant surgery is generally safe but does carry risks that require careful consideration. The most serious complication is infection, occurring in 1-3% of cases despite antibiotic-impregnated devices and strict sterile technique. Infection usually requires device removal, antibiotic treatment, and delayed reimplantation after 3-6 months—devastating for patients but fortunately rare. Mechanical failure (device malfunction) occurs in approximately 5-10% of inflatable devices over 10-15 years, requiring replacement surgery. Other complications include erosion (device breaking through tissue into urethra or skin—requires removal, occurring in <1-2%), chronic pain beyond expected recovery period (rare but may require device removal), unsatisfactory cosmetic result (size concerns, asymmetry—can sometimes be revised), and partner dissatisfaction (emphasizing importance of pre-operative couple counseling). Specific surgical risks include bleeding, hematoma formation, injury to urethra or bladder (rare), and anesthesia complications. Dr. Singh’s extensive experience, use of antibiotic-coated devices, and meticulous surgical technique minimize these risks substantially. Despite these potential complications, patient satisfaction remains very high (>90%) because the benefits typically far outweigh the risks for men with severe, refractory ED.
Modern penile prostheses are remarkably durable. Current generation three-piece inflatable devices have mechanical survival rates (device still functioning) of approximately 90-95% at 5 years, 85-90% at 10 years, and 70-80% at 15 years. Semi-rigid implants typically last even longer due to simpler design with no mechanical parts to fail—often 15-20+ years. When mechanical failure occurs with inflatables, it’s usually due to fluid leak, pump failure, or cylinder problems—the device doesn’t suddenly “break” but gradually loses function (incomplete inflation, difficulty deflating, or fluid leakage). If failure occurs, revision surgery to replace the device is straightforward and usually successful, as the implant space is already established. Most men who need revision due to mechanical failure choose to have another implant placed rather than return to non-surgical ED treatments, indicating high satisfaction even with this complication. Modern devices also come with manufacturer warranties (typically 5 years) covering replacement costs if mechanical failure occurs, though surgical fees still apply. Dr. Singh provides lifelong follow-up, monitoring device function and addressing any concerns promptly.
This is a common and important concern. Most patients maintain their pre-erectile dysfunction erect size with implants—the device is custom-sized during surgery to fit your individual anatomy. However, several factors affect perceived size outcomes. If ED has been present for many years, some tissue atrophy (shrinkage) may have already occurred, making the flaccid and erect penis smaller than remembered from younger years—the implant restores current anatomical size, not size from decades ago. Semi-rigid implants may result in slight length reduction compared to best natural erections because they’re sized conservatively to prevent erosion. Three-piece inflatable devices typically provide best length outcomes because they can be sized more aggressively and provide maximum expansion. Some patients undergo concurrent penile lengthening procedures if significant shortening has occurred. Girth usually remains unchanged or may slightly increase with implants. It’s crucial to have realistic expectations—implants restore erectile function but don’t increase size beyond your natural anatomy. Dr. Singh provides honest assessment during consultation about expected size outcomes. Most patients adjust well and prioritize reliable function over size concerns, especially after years of ED-related distress.
Sexual activity must be completely avoided for 6-8 weeks post-surgery to allow complete healing of surgical sites and device integration into tissues. Premature sexual activity risks serious complications, including infection, device malposition, erosion, or mechanical damage. The timeline breaks down as follows: Weeks 0-4 involve primary healing—incisions closing, swelling resolving, tissues adapting to the device. Any sexual activity or even erections are prohibited. Weeks 4-6 see continued tissue maturation and device encapsulation by the body—device remains deactivated. Week 6-8 is when Dr. Singh evaluates healing and teaches device operation during the office visit. Once cleared, you’ll practice inflating/deflating for 1-2 weeks to become comfortable. Sexual activity can begin 6-8 weeks post-surgery once healing is confirmed, starting gently and gradually increasing intensity. Expect an adjustment period of 2-3 months—initial attempts may feel awkward or mechanical, psychological adjustment takes time, and you and your partner need to learn optimal techniques. Most couples report that by 3-6 months, sexual activity feels natural and satisfying. Counseling or sex therapy can help during this adjustment period. Patience and communication with your partner are essential for optimal outcomes and relationship satisfaction.
The leading center for advanced, compassionate urological care and treatment in Indore, Madhya Pradesh.