Dr. Vikas Singh is a highly accomplished Consultant Urologist in Indore, specializing in advanced surgical reconstruction for complex Urethral Stricture Disease. With extensive training and experience in both endoscopic and open reconstructive urology, he offers comprehensive urethroplasty procedures—the definitive surgical solution for recurrent, long, or complex urethral strictures. His expertise encompasses the full spectrum of reconstructive techniques including anastomotic urethroplasty, buccal mucosal graft urethroplasty, penile skin flap procedures, and staged reconstructions for the most challenging cases. Practicing at Kokilaben Dhirubhai Ambani Hospital Indore with access to specialized microsurgical instruments and multidisciplinary support, Dr. Singh achieves success rates exceeding 85-95%—offering patients a genuine cure rather than temporary relief. His approach prioritizes not only stricture resolution but also preservation of urinary continence, sexual function, and cosmetic outcomes. We maintain complete transparency regarding treatment costs and provide comprehensive insurance assistance for our patients across Central India.
Consultant Surgeon at Kokilaben Dhirubhai Ambani Hospital, Indore, with specialized reconstructive surgery capabilities.
Extensive expertise in complex urethral reconstruction with hundreds of successful urethroplasty procedures.
Exceptional long-term success rates with minimal recurrence—true cure for most patients.
Unlike endoscopic procedures (OIU/Laser) that simply cut through scar tissue with high recurrence rates (40-60%), urethroplasty is open reconstructive surgery that removes or replaces the diseased urethral segment. By excising scar tissue and reconstructing with healthy tissue, it addresses the root problem rather than providing temporary relief. This results in dramatically superior long-term success rates of 85-95% with minimal recurrence.
Urethroplasty becomes the treatment of choice for recurrent strictures (failed one or more OIUs), long strictures (>1.5-2 cm), complete obliterations (no passage), complex strictures involving multiple segments, strictures caused by lichen sclerosus, or pan-urethral disease. It's also increasingly offered as first-line treatment for appropriate candidates seeking definitive cure rather than accepting repeated procedures and potential complications.
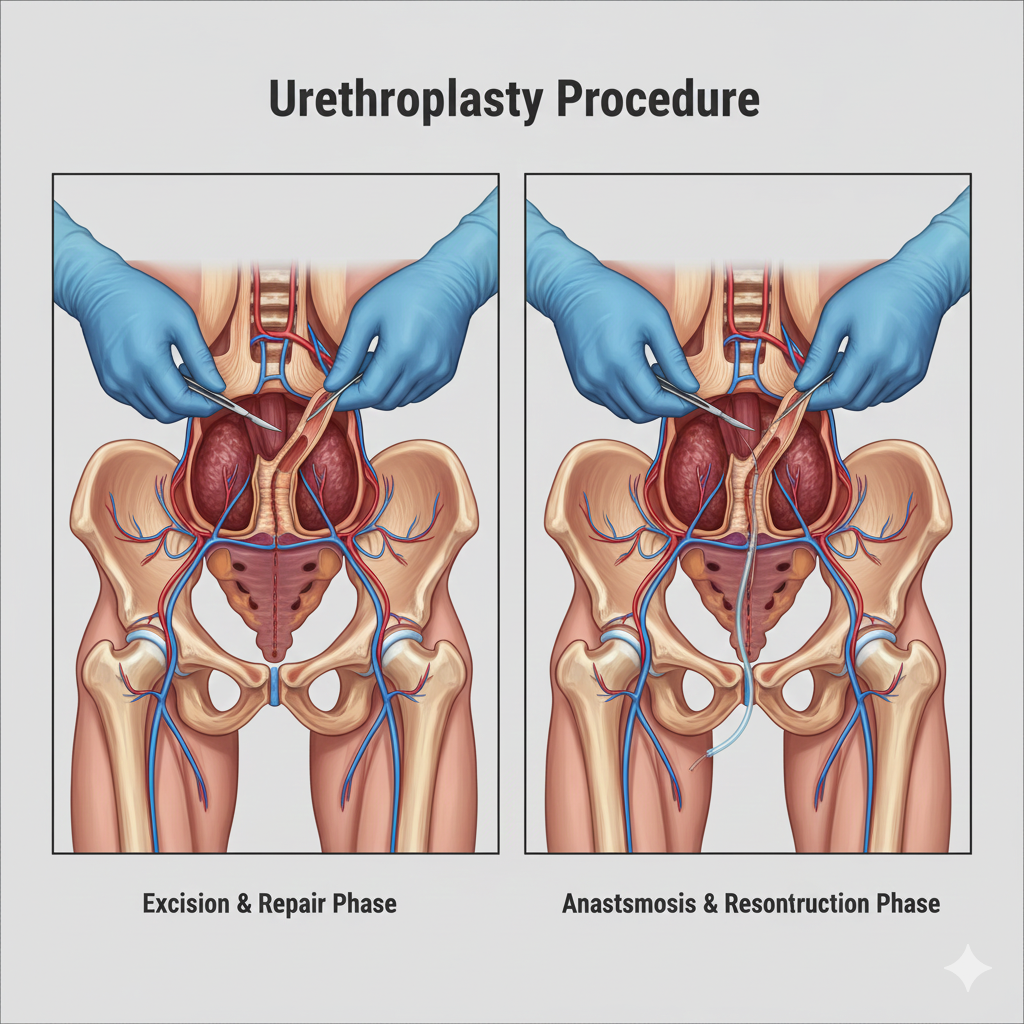
The technique selected depends on stricture location, length, and tissue quality. Anastomotic (excision and primary reanastomosis) involves removing the scarred segment and reconnecting healthy ends—ideal for short bulbar strictures. Augmented urethroplasty uses grafts (typically buccal mucosa from inside cheek) or flaps (penile or scrotal skin) to widen the narrowed segment—used for longer strictures. Staged urethroplasty involves multiple operations for extensive disease—first creating a urethral plate, then tubularizing it months later.
This technique is ideal for short bulbar strictures (<2 cm). The diseased urethral segment is completely excised, and the two healthy ends are spatulated (opened wider) and sutured together with fine absorbable sutures. This provides the highest success rates (95%+) because all scar tissue is removed. The procedure requires careful mobilization of the urethra to achieve tension-free reconnection. Recovery involves catheterization for 2-3 weeks. Best For: Short (<2 cm) bulbar strictures; highest success rate technique.
For longer strictures (>2 cm) where excision isn’t feasible, augmentation with buccal mucosa (tissue from inside cheek or lip) is the gold standard. The strictured segment is opened longitudinally, and a patch of buccal mucosa is harvested and quilted into place to widen the urethra. Buccal mucosa is ideal because it’s resilient, takes well in the urethral environment, has good blood supply, and heals with minimal scarring. The oral donor site heals completely within 2-3 weeks with minimal discomfort. Best For: Longer strictures (>2 cm), anterior urethral strictures, lichen sclerosus cases.
When strictures involve the penile urethra or when buccal mucosa isn’t available, penile or scrotal skin flaps can be used. These local flaps maintain their own blood supply, providing excellent healing. Techniques include dorsal onlay grafts or ventral approaches depending on stricture characteristics. These procedures are more complex and require meticulous technique to preserve cosmetic appearance and function. Best For: Penile urethral strictures, cases where buccal mucosa is contraindicated or insufficient.
Comprehensive evaluation includes retrograde urethrography and voiding cystourethrography (X-ray studies defining stricture precisely), cystourethroscopy (direct visualization), uroflowmetry (measuring flow rate), and sometimes MRI for complex cases. These studies help Dr. Singh plan the exact surgical approach. Pre-operative counseling covers realistic expectations, potential complications, and functional outcomes.
Performed under spinal or general anesthesia, surgery typically takes 2-4 hours depending on complexity. A perineal incision (between scrotum and anus) is made for bulbar strictures, or a penile incision for anterior strictures. The urethra is carefully exposed, the strictured segment identified, and the chosen reconstructive technique performed using microsurgical suturing. A catheter and sometimes a suprapubic tube (temporary bladder drainage through lower abdomen) are placed.
Hospital stay is typically 2-4 days. The urethral catheter remains for 2-3 weeks to allow healing without urine flowing through the reconstruction. Some surgeons also place a suprapubic catheter as backup. Pain is managed with oral medications and is generally moderate and well-controlled. Before catheter removal, a pericatheter urethrogram (contrast X-ray) confirms adequate healing without leaks.
Success rates of 85-95% mean most patients achieve permanent resolution with a single surgery no more repeated procedures.
Return to normal urination, elimination of recurrent infections, improved bladder emptying, and freedom from catheterizations.
When performed expertly, urethroplasty preserves erectile function, ejaculatory function, and urinary continence in vast majority of patients.
Unlike endoscopic procedures with high recurrence, successful urethroplasty typically provides lifelong resolution of stricture disease.
Schedule a private, confidential consultation with Dr. Singh in Indore.
The decision depends on your stricture history and characteristics. If you’ve already had 1-2 failed endoscopic treatments (OIU, dilation, or laser), continuing with repeated procedures has very low success rates (often <30%) and actually makes the stricture worse by creating more scar tissue. Studies show that after two failed endoscopic treatments, the chance of success with a third attempt is minimal, while surgical complications increase. Similarly, if your stricture is long (>2 cm), involves multiple segments, or is caused by lichen sclerosus (inflammatory condition), endoscopic approaches have poor outcomes from the start. In these situations, urethroplasty offers 85-95% cure rates versus accepting endless cycles of temporary relief followed by recurrence. Dr. Singh will review your imaging, treatment history, and symptom severity to provide honest guidance on whether another endoscopic attempt is reasonable or if it’s time for definitive reconstruction that actually solves the problem.
Urethroplasty success rates are excellent and depend on stricture location and technique used. Anastomotic urethroplasty (excision and reconnection) for short bulbar strictures achieves success rates of 95%+ in experienced hands. Augmented urethroplasty with buccal mucosal grafts for longer strictures succeeds in 85-90% of cases. Even complex penile strictures have 75-85% success rates with appropriate techniques. “Success” means maintaining adequate urinary flow without need for further intervention. Most recurrences occur within the first year if they happen at all—after 12-18 months of good flow, the likelihood of late failure is very low. Many patients enjoy 10, 20, or more years of excellent function after successful urethroplasty. This durability far exceeds endoscopic procedures where recurrence is expected in 40-60% of cases within months to years. The investment in a more complex surgery yields dramatically superior long-term outcomes.
Preservation of sexual function is a primary priority in urethroplasty. When performed by experienced surgeons using proper technique, erectile function is preserved in 90-95% of patients because the surgery is performed on the urethra, carefully avoiding injury to the adjacent erectile tissue (corpus cavernosum) and the nerves/blood vessels responsible for erections. Ejaculatory function is similarly preserved in the vast majority. Temporary changes are common—some men notice decreased rigidity or delayed ejaculation for 2-3 months post-surgery, but this typically resolves completely by 6 months. For fertility, sperm quality and production aren’t affected as the surgery doesn’t involve the testicles or vas deferens. The most important factor is surgeon experience—meticulous dissection technique protecting the delicate structures around the urethra. Dr. Singh’s extensive training in reconstructive urology ensures these critical functions are safeguarded while achieving stricture cure.
Buccal mucosa is the moist inner lining of your cheek or lower lip—the same tissue that lines your entire mouth. It’s ideal for urethral reconstruction because it’s naturally suited to a moist environment, has excellent blood supply, heals with minimal scarring, and is resistant to infection. During surgery, a strip of tissue (typically 4-6 cm long by 1.5 cm wide) is carefully harvested from inside your cheek under the same anesthesia as the urethroplasty. The donor site is left to heal naturally or sometimes closed with absorbable sutures. Post-operative oral care is simple: soft diet for 3-5 days, salt water rinses, and avoiding spicy foods. Most patients report the oral donor site is less bothersome than the perineal surgical site. The mouth heals completely within 2-3 weeks with no visible scarring, minimal functional impact, and no long-term issues with eating, speaking, or oral hygiene. In rare cases where very long strictures require extensive grafting, both cheeks can be harvested without significant morbidity.
Pain after urethroplasty is moderate and highly variable between patients. The perineal incision causes more discomfort than the urethral reconstruction itself. Most patients describe it as a deep aching or pressure sensation, particularly when sitting, rather than sharp pain. Hospital pain management includes IV medications initially, transitioning to oral pain relievers before discharge. At home, most patients need prescription pain medication for 5-7 days, then over-the-counter medications suffice. Sitting on a donut cushion helps comfort. The catheter itself causes bladder spasms (sudden urge sensations) managed with anticholinergic medications. Overall recovery timeline: 2-4 days hospitalized, 2-3 weeks with catheter restricting activities, 4-6 weeks before returning to work (desk jobs earlier, physical labor later), and 8-12 weeks before full recovery including strenuous exercise and sexual activity. While more involved than endoscopic procedures, the recovery is very manageable, and most patients feel the temporary discomfort is well worth achieving permanent cure.
Urethroplasty is generally safe but does carry surgical risks that should be understood. Common minor issues include temporary urinary urgency or frequency (usually resolves within 3 months), mild urinary spraying requiring seated voiding initially (improves over time), and wound discomfort during healing. More significant complications occur in <5-10% of cases and include urethrocutaneous fistula (abnormal connection between urethra and skin causing urine leak, often requiring minor surgical repair), urinary tract infection (treated with antibiotics), hematoma or bleeding requiring drainage, and stricture recurrence requiring additional treatment. Serious complications affecting sexual function (erectile dysfunction, ejaculatory problems) are rare (<5%) when surgery is performed expertly. Other rare risks include injury to rectum (if dissection extends too deep) or suprapubic catheter complications. Dr. Singh’s extensive experience minimizes these risks, and comprehensive pre-operative counseling ensures you understand and can make informed decisions about accepting these risks versus living with untreated stricture disease.
The leading center for advanced, compassionate urological care and treatment in Indore, Madhya Pradesh.