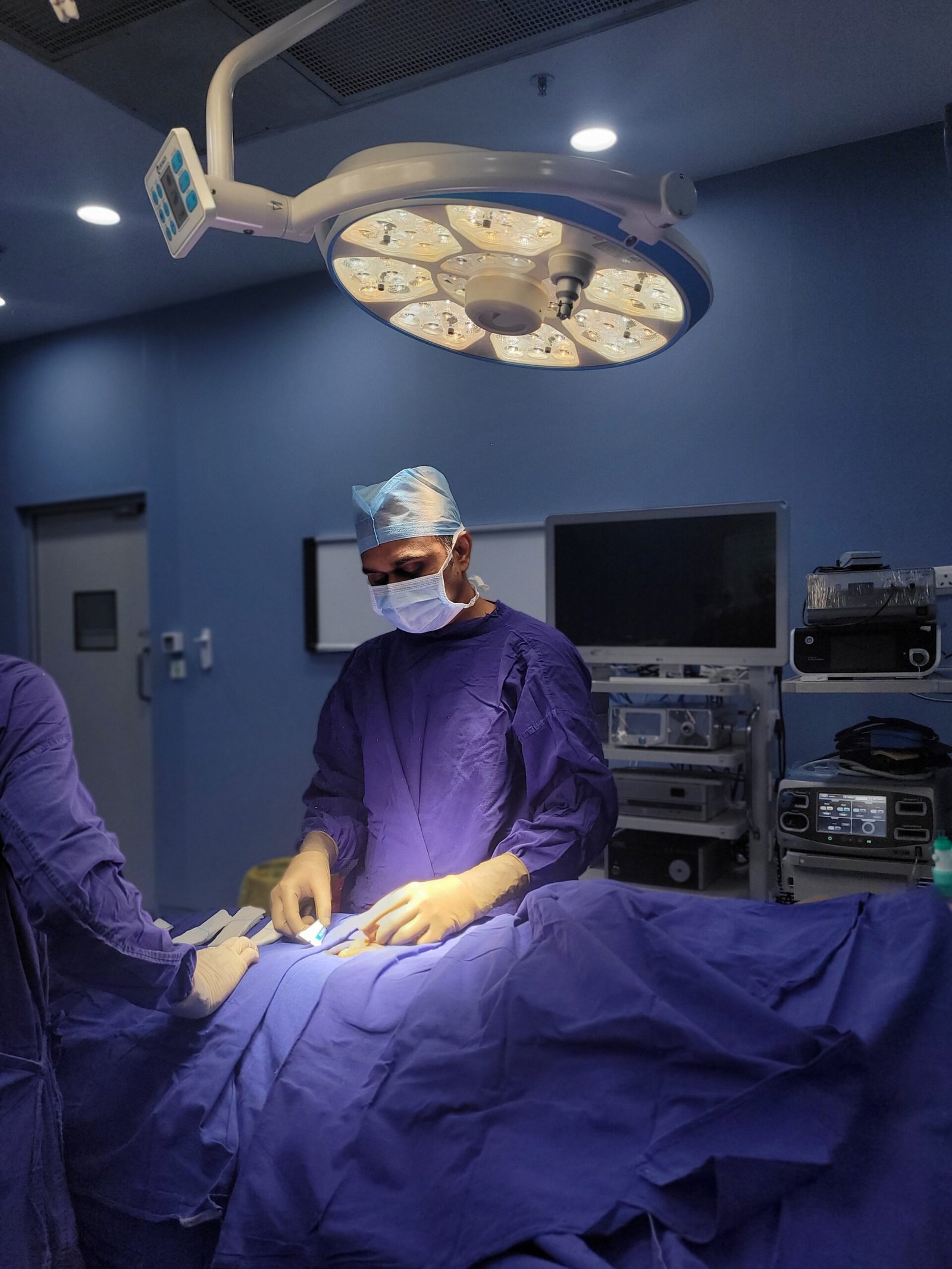
Kidney stones are as tough as it gets and get even tougher when your stone is large and stubborn making you choose between painful procedures. Thankfully, RIRS helps you avoid tough situations.
RIRS is the advanced and most painless option that currently exists for laser kidney stone treatments. A camera about the shape and length of a pencil is used and maneuvers through the passages of your body to get to your kidney. A laser is then used to pulverize the stone into dust. The best part? You’re home the next day and there is not a single scar or mark or cut or stitch on your body. It’s essentially surgery without the surgery.
RIRS stands for Retrograde Intrarenal Surgery. Let us break that down:
Retrograde means backwards. For the purpose of this procedure, it means up the urinary tract, starting at the urethral opening, going into the bladder, up the ureter, and ending at the kidney (The approach is from the inside, rather than the outside of the body).
Intrarenal means inside the kidney. This is most likely where the stone is.
Surgery: This procedure is performed from the body’s natural urinary paths, so an incision RIRS does not involve an incision.
The preferred, non-invasive therapy for treating kidney stones comes from a thin, flexible, and minimally liner RIRS telescope which is guided through the urethra and then the entire urinary system to the location of the kidney stone, a laser is then sent through the previously mentioned telescope to break the kidney stones to smaller fragments which are later excreted through urine and fully removed from the body. This therapy is completely scar and incision free as it naturally sent guided down reverse of the standard urine path.
It is now the most popular treatment for kidney stones that are part of the 1 cm to 2.5 cm range. It is a preferred therapy for stones that are less accessible – e.g. located in the lower pole of the kidney and stones that are larger than 3 cm – as long as it is in conjunction with PCNL.
The flexible ureteroscope is a great medical innovation. It is a tube of fiber optics 3 to 4 mm in diameter, containing a high definition camera on the tip. This camera sends a live stream of a magnified image to a monitor in the operating room. The unique aspect of the flexible ureteroscope is that the distal tip can be deflected 270 degrees in either direction. Therefore, surgeons can “steer” the ureteroscope to each calyx in the kidney to obtain a complete view of the kidney.
A flexible ureteroscope travels through the urethra, bladder, and ureter to get to the kidney, in the pathway of the body’s natural urinary system. As the ureter (3 to 4 mm in diameter) is too narrow to let a flexible ureteroscope pass, a ureteral access sheath (thin plastic pipe) is placed in the ureter to keep it open. A flexible ureteroscope can then pass through. The tip can be deflected to go to a calyx where a stone is located.
This entire process is done using real-time video. Dr. Vikas Singh uses this video to guide the ureteroscope. This makes it easier to figure out where the ureteroscope should go. To keep the view clear and flush the area, saline is run through the ureteroscope. Once the stone is located, a laser is used, and the laser fiber is placed.
After the flexible ureteroscope navigates to the location of the stone, a fiber optic laser with a diameter of 200-365 microns, which is even thinner than a single strand of hair, is inserted through the operative channel of the ureteroscope to the stone’s surface.
The laser is then switched on when it comes to the Holmium. The Holmium is the benchmark laser for the treatment of kidney stones. This laser is capable of fragmenting any stone, regardless of the stone’s composition of calcium oxalate, uric acid, struvite, or cystine. This is done through the destruction of the stone’s mineral structure. When the Holmium laser is directed at the stone, the edge of laser line turns the mineral particles into microscopic fragments, and through the heat of the laser, ‘dust’ heats these tiny particles to the point that they vapor collect into gas.
Utilizing this ‘dust and flush’ concept, Dr. Vikas Singh, does this linearly, as the laser is then swept to convert the stone, rather than into large pieces, to finer to vapor. Once in the diluted ‘dust’, it is then much finer than (less than) 0.1 mm, and slowly ‘flushed’ out with the inter-procedure irrigation fluid and later on, post-surgery, with regular urine. Assuming the pieces have even momentarily broken into ‘dust’, in most instances, there are not any pieces that need to be retrieved with baskets. In this instance, the stone’s vaporization into dust is complete.
Contemporary systems incorporating MOSES Holmium cutting-edge technology fragmented stones of various sizes in 30-90 minute time spans with fine control of energy distribution per pulse and pulse frequency. Unlike traditional lasers, Holmium’s energy is entirely absorbed by the stones and is very safe as it protects the renal tissues.
RIRS has excellent advantages when treating patients with multiple small stones located at different levels in all compartments of the kidney, as the flexible ureteroscope can reach every calyx in the kidney and the stones can be treated with the laser in different sessions. This is a distinct benefit over PCNL and stones left untreated in certain inaccessible calyces, and above ESWL in that it can take multiple sessions and break the stones to leave fragments, which still need to be treated.
RIRS can be employed in both kidneys in one sitting in select patients with either of the multiple small stone distributions resembling nephrocalcinosis, bilateral renal stones, or nephrocalcinosis. This would significantly lessen the burden/component of multiple treatment surgeries for the patient.
RIRS is popular with patients as it is performed entirely without making an incision, cut, or puncture in the skin, and therefore it does not result in any external marking or scarring on the body. During the RIRS procedure, the urinary tract is entered and worked on through the body’s own urinary orifice. Therefore, the body’s skin remains altogether intact, and there is no external evidence of any urinary tract surgery on the body.
Scar, incision, or cut concerns become less important with less invasive surgeries. For those who may have an injury or wound incision complications, especially with external hernias, RIRS is ideal. Those who are planned to have some type of body surgery whose job complicates scarring, or who are concerned about the harm irregularities or scarring may do, RIRS is the less invasive solution.
RIRS is typically recommended for stones that are between 1 cm and 2.5 cm. For stones that are below 1 cm, they are able to be treated by drinking a lot of fluids or by taking medications. However, RIRS is also a good option for renal stones that are not passing and have stuck and/or caused pain or infected renal stones. For stones that are more than 2.5 cm, the PCNL procedure is offered, which is a back incision to remove the stones. 3 cm stones are around the top end of RIRS, and in some clinics, RIRS is the procedure for up to 4 cm stones.
RIRS is the preferred procedure for stones that are between 1 cm and 2.5 cm because it is successful in more than 85% of the operations, and sometimes RIRS is successful for even more than 95% of the patients. Naturally, RIRS is the procedure that is done at Kokilaben Hospital for most clients who fall in this range. Dr. Vikas Singh is an expert at assessing the dimensions and assortment distribution of the stones by analyzing the client’s data from the CT scan, in particular the image segments called Hounsfield units, to decide if the RIRS procedure would be the best solution for his stones.
The biggest indicator of having a kidney stone is renal colic. Renal colic is a sudden onset of a relentless cramping pain that starts at the flank and back. Renal colic pain is likely to develop at the back of the flank and at the back and the sides of the rib cage, then, radiate over to the scrotum, pubis, and tested to the inner thigh pain as the kidney stones travels down the ureter and out of the body. This pain is likely to develop waves. Renal colic pain is so tremendous that it is likely to induce nausea and vomiting. People having renal colic pain have stated that it is the worst pain Ever, that they have Ever experience. If you are experiencing persistent pain and especially, if it is getting more worse, you very likely have kidney stones, so you should get and likely to require a immediate medical care.
Either gross or microscopic hematuria, or blood in the urine, is an indication of the presence of kidney stones. Due to the abrasive and sharp nature of nephroliths, as the stones travel down the urinary tract, hematuria is likely as they rub against the lining of the ureter or the collecting system of the kidney. Even a single painless episode of hematuria should be the subject of a timely investigation by urologists. Even though most often it is due to the presence of nephroliths, a urologist must eliminate the presence of bladder or kidney cancers before a proper diagnosis is made.
A kidney stone that is in the lower ureteral segment can produce UTI-like symptoms. For example, there can be an urgent, increased frequency of urination and a burning pain that occurs when urinating. Some patients, in fact, receive treatment for a UTI before the kidney stone is discovered. If a patient is enduring UTI symptoms after antibiotic treatment, or after an antibiotic for UTI symptoms has been taken and the symptoms return shortly after, or the UTI is known to be resistant or has been diagnosed to be refractory, a stone in the urinary tract may be of the highest suspicion, and a urological consultation should be conducted.
Here is a clear comparison of RIRS against the main alternative kidney stone treatment options:
Factor | RIRS | PCNL | ESWL (Shockwave) |
External Incision | None – completely through urethra | 1cm keyhole incision in back | None – external shockwaves |
Anaesthesia | General or spinal | General or spinal | Local or sedation (no anaesthesia in some) |
Stone Size | Best for 1–2.5 cm | Best for >2 cm | Best for <1.5 cm |
Stone-Free Rate | 85–95% in 1 session | 90–95% in 1 session | 50–80% (may need repeat) |
All Kidney Locations | Yes – flexible scope reaches everywhere | Limited – depends on access tract | Limited – some poles less effective |
Hospital Stay | 1–2 days | 2–3 days | Day procedure |
Blood Loss | None (no incision) | Small amount possible | None |
Recovery | 5–7 days | 1–2 weeks | 1–3 days |
Suitable for Hard Stones | Yes – Holmium laser treats all types | Yes | Limited – may fail on very hard stones |
Bilateral (Both Kidneys) | Possible in same session | Separate sessions needed | Possible |
RIRS is the only kidney stone procedure that doesn’t leave any external marks on the body. The skin remains uncut. No tool is inserted through the body wall. No stitches are necessary. The ureteroscope passes through the urethra, the body’s natural urinary pathway, and exits the same way. There are patients who are worried about the leaving scars and external wound complications as a result of surgery, and with RIRS their worries are fully eliminated. The only external change that can be noticed on the day after the RIRS surgery from the day before is that a small catheter that has a urine bag, which is removed before the patient leaves the hospital.
One key benefit that RIRS offers that older techniques don’t is that RIRS can treat stones in any calyx in the kidney, even the difficult-to-reach lower pole calyx. RIRS is a technique that uses a flexible ureteroscope. The flexible ureteroscope tip can deflect 270 degrees. This makes it possible for the flexible ureteroscope to access the lower pole calyx, even the difficult-to-reach ones. ESWL is even less effective for stones in the lower pole and clinical studies consistently show that shockwave lithotripsy for lower pole stones are less likely to become stone-free compared to other positions in the kidney. RIRS is as effective in this case compared to other positions in the kidney.
Since no tissues are severed and no blood vessels are breached, RIRS results in no blood loss. There are no sutures to remove, and the body heals from RIRS much more quickly than after treatment by its main competitor for stones of medium size, PCNL. RIRS patients are able to move and feel comfortable just hours after anesthesia, and leave the hospital the day after. Light work can resume in 3 to 5 days. This must be compared to PCNL, where the need for a kidney cut means a recovery of 1 to 2 weeks with restricted activity.
At Kokilaben Hospital in Indore, the RIRS procedure takes about a day. Most patients come in the day before and leave the day after. Shorter stone cases, leave patients able to go home within the same day. Shorter surgeries allow less disruption to personal lives and fewer costs to patients.
RIRS has an excellent safety profile. When performed by an experienced surgeon, RIRS is one of the safest urological procedures. That said, patients should know the potential side effects of every procedure they are going to undergo. Dr. Vikas Singh does discuss these side effects in detail during the pre-procedure consultation.
Day of Surgery: RIRS is performed with general or spinal anesthesia. During the surgery, you’re ‘asleep’ or ‘numb’ below the waist. RIRS takes about 30 to 90 minutes, depending on the size and complexity of the stones. A DJ stent is placed at the end of the RIRS. After the procedure, you will be in recovery and will have a urinary catheter and IV saline drip. Mild discomfort is common, but is managed with oral pain relief.
The urinary catheter is usually taken out in the morning. After the removal of the catheter most patients urinate well. Blood tinged urine is common and expected. The nursing team prepares for discharge after confirming patients are urinating satisfactorily, are taking in an acceptable amount of oral fluids, and are in acceptable amounts of pain. Patients are usually home from the hospital by early afternoon on day 1.
Aim to drink 2.5 to 3 litres of water each day. This helps with washing urine based fine stone dust out of the urinary tract. It is normal to have blood tinged urine for a week. Slight urinary frequency, urgency, or pain in the flank or lower abdomen because of the stent, will continue. You should take all of the prescribed medications, which include antibiotics, anti-inflammatories, and alpha-blockers (for example, tamsulosin, which helps with pain and discomfort). When it comes to work, possible to return to since 3 to 5 days after the procedure. The DJ stent is expected to be removed, at which point, you can resume all normal activities including strenuous exercise, heavy lifting, and sexual intercourse.
A DJ stent removal usually happens between 1 to 4 weeks after an RIRS, adjusted according to your case by Dr. Vikas Singh. Many start to feel better instantly after removal. Side effects such as urgency, frequency, and flank discomfort go away quickly. There are no restrictions put in place after the removal that would prevent someone from doing anything in their regular daily routine.
To determine if the kidney is free of stone or if there are small stone fragments remaining, a CT scan or an ultrasound is performed. A urine analysis is done to rule out infection. Dr. Vikas Singh will also address prevention of kidney stones i.e. changes to diet, fluid intake, and any risks of metabolism noted in the blood and urine tests to determine the risk of developing kidney stones in the future.
RIRS can be done using general anesthesia or spinal anesthesia. This means that there isn’t any feeling during the procedure. After the procedure you may experience some urinary discomfort, stinging during urination, and flank discomfort. You may expect discomfort from the DJ stent from 1- 2 weeks. Most patients have described discomfort from the procedure to be more comfortable than the pain coming from the kidney stones. Pain relief from any discomfort can be managed by standard oral pain relief medications.
Factors that affect the time spent include the stones’ number, size, and location, and the complexity of the given case. RIRS that involves one stone of size 10 to 15mm usually lasts 45 to 75 minutes. Stones that are larger or that are present in greater numbers may last 90 minutes to 2 hours. A specific estimate that your doctor will give during the pre-procedure consultation will be based on your CT scan.
New stones in the kidney are independent from the first one and are formed de novo meaning they aren’t just a residual portion of the first stone. RIRS can be repeated if there was a formation of a new kidney stone in the future because this procedure can be done without restrictions. The most crucial thing in reducing the frequency of stone development is determining the source of your stone from a metabolic perspective and then adapting relevant lifestyle and dietary changes.
RIRS and URS (ureteroscopy) are techniques involving the use of a telescope to access the urinary tract to remove urinary stones. The primary difference is the type of technology. URS is mainly the use of a semi-rigid ureteroscope, which can only access the ureter and the renal pelvis; it can’t go into the calyces. RIRS uses a fully flexible ureteroscope, which can go up to 270 degrees and are able to access all parts of the kidney, including all the calyces. That makes RIRS ideal for stones that lie in the kidney, and URS for those in the ureter.
Neither of the methods stands out as the superior technique, as both methods focus on solving the stones with different sizes and circumstances. RIRS is indicated for stones with sizes from 2 to 2.5 cm, stones located in the lower pole, and for treatment to be scarless, and for patients who have altered lower pole/pelvic scarring making PCNL unsafe. PCNL is indicated for stones of sizes 2 to 3 cm, staghorn calculi, and for treatment to be completed in one round with a high stone-free rate. In most cases both PCNL and RIRS can be combined, with PCNL being done first to disintegrate the main bulk of the stones, and followed by RIRS to complete the treatment. Dr. Vikas Singh is skilled in both methods, and will be able to give correct advice for your stones.
The period for the DJ stent placement can be anywhere from 1 to 4 weeks, depending on the complication level of the RIRS, amount of ureteral injury, size of the fragments of the stone passing, and any preexisting infections. Dr. Vikas Singh will note how long the stent will remain for your case and will also make the appointment to have it removed once you leave the hospital.
Yes, RIRS in the same anesthetic session in both kidneys is possible in a select cohort with bilateral kidney stones. Taking advantage over PCNL, where bilateral treatment in a session is almost never the case, it is one of the practical advantages of RIRS. The operation should be decided considering the total amount of kidney stones, the patient’s health status and the expected duration of the operation. Draw Dr. Vikas Singh if the case RIRS should be done.
Fever after RIRS, especially if above 38°C, could be a sign of a urinary tract infection or, more severely, the development of urosepsis, which is the spread of infection to the bloodstream. You need to seek medical attention immediately. Call Dr. Vikas Singh or go to the Kokilaben Hospital emergency room. Do not assume the fever will go away on its own. Treatable infections after RIRS will typically be cleared using antibiotics; however, if infected, the situation could worsen quickly without medical attention.
Yes, one of the greatest ways to prevent the recurrence of kidney stones is to change your diet. General suggestions are to drink 2.5 to 3 litres of water a day, decrease your sodium (salt) consumption, reduce animal protein consumption, and if the stones are calcium oxalate based, avoid oxalate rich foods such as spinach, nuts, chocolate, and tea. There are more careful suggestions based on the stones, which is likely why Dr. Vikas Singh would ask to do a 24 hour urine collection and analyze the stones after your RIRS to understand the risks and then be able to devise a defence strategy for you.
24/7 Services Available
Copyright © 2026 Urology Center | All Rights Reserved
Design and Developed by Namastetu Technologies Pvt.Ltd