Dr. Vikas Singh is a highly specialized Consultant Urologist and Andrologist in Indore, offering comprehensive evaluation and advanced treatment for Peyronie’s Disease—a condition causing abnormal penile curvature, pain, and erectile dysfunction due to fibrous plaque formation. With extensive training in Andrology and male sexual medicine, he provides the complete spectrum of treatment options ranging from conservative medical management and minimally invasive injections to advanced surgical correction techniques including penile plication, plaque excision with grafting, and penile implants with modeling. Practicing at Kokilaben Dhirubhai Ambani Hospital Indore with access to specialized diagnostic equipment, injection therapies, and microsurgical capabilities, Dr. Singh tailors treatment to disease stage, severity of curvature, and patient goals. His compassionate, judgment-free approach ensures comfortable discussions about this sensitive condition, realistic treatment expectations, and comprehensive support throughout the treatment journey. We maintain complete confidentiality and transparency regarding treatment costs for our patients across Central India.
Consultant Surgeon at Kokilaben Dhirubhai Ambani Hospital, Indore, with specialized andrology and reconstructive capabilities.
Advanced fellowship in male sexual medicine including comprehensive Peyronie's disease management and surgical correction.
Treatment customized to disease stage, curvature severity, erectile function status, and individual patient goals.
Peyronie's Disease is a connective tissue disorder affecting the penis, characterized by development of fibrous scar tissue (plaque) within the tunica albuginea—the thick sheath surrounding the erectile chambers. This plaque causes penile curvature (upward, downward, or lateral), shortening, narrowing (hourglass deformity), painful erections, and often erectile dysfunction. The condition typically develops gradually and can significantly impact sexual function, self-esteem, and relationships.
While the exact cause remains unclear, Peyronie's likely results from repeated minor trauma during sexual activity or injury causing internal bleeding and inflammation. Risk factors include genetic predisposition (family history), age (most common 40-60 years), connective tissue disorders (Dupuytren's contracture), diabetes, smoking, and certain medications. Not all men with these risk factors develop Peyronie's, suggesting multiple contributing factors.
Peyronie's progresses through two distinct phases: The Acute/Active Phase (6-18 months) involves ongoing inflammation, progressive curvature development, painful erections, and plaque formation—this is when medical treatments may slow progression. The Chronic/Stable Phase occurs when curvature stabilizes (no change for 3-6 months), pain resolves, plaque calcifies and hardens—this is when surgical correction becomes appropriate if needed. Understanding disease stage is critical for treatment selection.
For early-stage disease, conservative treatments aim to reduce inflammation, prevent progression, and promote plaque resolution. Options include oral medications (Vitamin E, Potaba, colchicine, pentoxifylline—modest evidence, minimal side effects), topical verapamil gel, vacuum erection devices to prevent shortening, and penile traction therapy (controlled stretching to counteract curvature). While these treatments show limited definitive evidence, they may benefit some patients with mild disease and are worth trying during the acute phase before considering more invasive options.
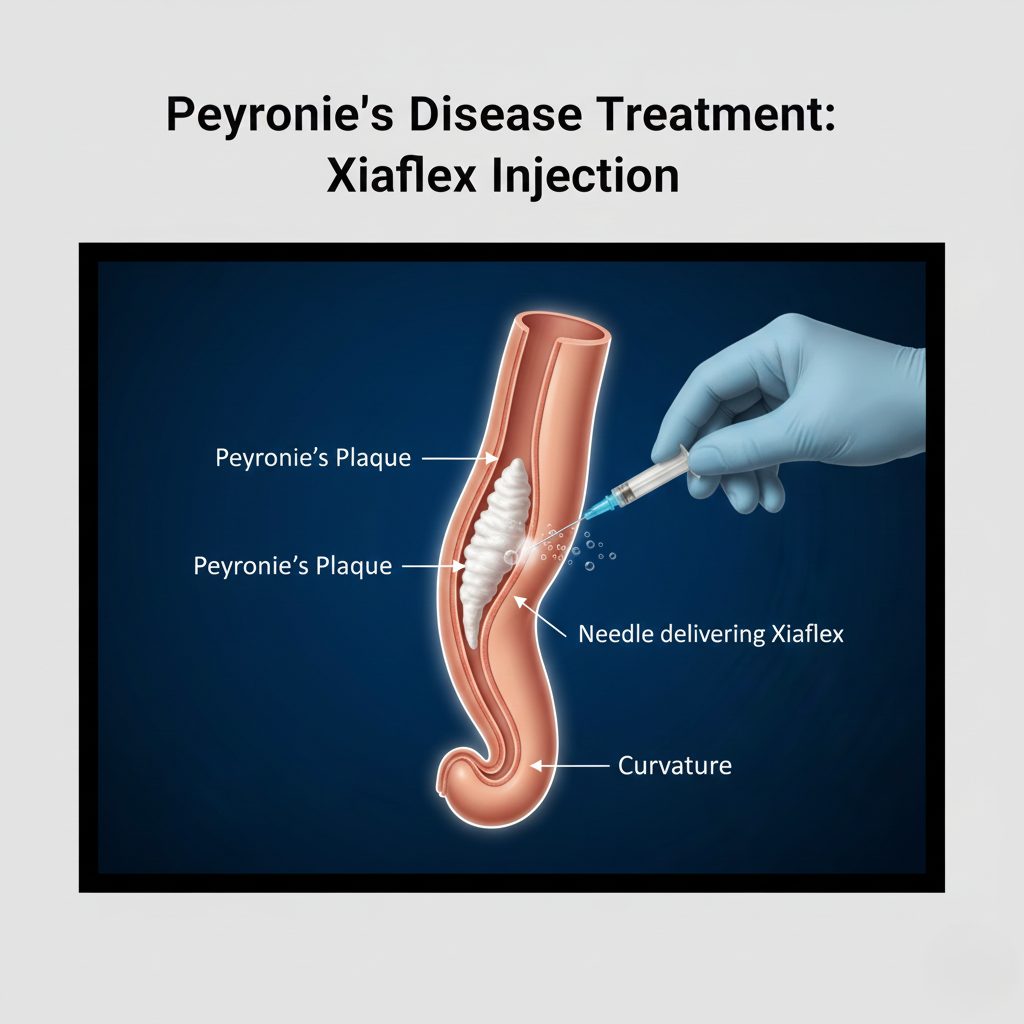
Injectable treatments delivered directly into the plaque offer more targeted therapy. Collagenase Clostridium Histolyticum (Xiaflex) is FDA-approved specifically for Peyronie’s, works by breaking down collagen in plaques, requires multiple injection cycles, and reduces curvature by 30-40% on average—best for curvatures 30-90 degrees without severe ED. Verapamil injections (calcium channel blocker) may reduce plaque size and pain, though evidence is less robust. Interferon injections reduce inflammation and fibrosis but are expensive with limited availability. Dr. Singh administers injections in-office with minimal discomfort and monitors response over multiple treatment cycles.
When curvature is severe (>60 degrees), prevents intercourse, or causes significant distress after disease stabilization, surgical correction offers definitive solutions. Three main approaches exist: Penile Plication (shortening the longer side to match the curved side—simple, preserves erectile function, ideal for curvatures <60 degrees without ED), Plaque Incision/Excision with Grafting (lengthening the shorter side by cutting plaque and placing graft material—for severe curvature >60 degrees, more complex, slight ED risk), and Penile Implant with Modeling (for men with both Peyronie’s and severe ED—addresses both problems simultaneously). Dr. Singh selects the optimal technique based on curvature severity, erectile function, penile length, and patient priorities.
This straightforward technique involves placing permanent sutures on the longer (convex) side of the penis opposite the plaque to create shortening that matches the curved side, resulting in straightening. Advantages include simple procedure (60-90 minutes), preserves erectile function (no plaque manipulation), low complication risk, outpatient surgery with quick recovery, and excellent straightening results for appropriate candidates. Disadvantages include penile shortening (typically 1-2 cm), not suitable for severe curvatures >60 degrees, and potential for suture palpability. Best for patients with good erectile function, moderate curvature 30-60 degrees, adequate length to tolerate some shortening, and prioritizing simplicity and function preservation. Primary Advantages: Simplest surgery, preserves erections, quick recovery, excellent outcomes for appropriate cases.
More complex technique involving incising or removing the plaque and placing a graft (typically from pericardium, dermis, or synthetic materials) to lengthen the shortened side. Advantages include treats severe curvatures >60 degrees, preserves or improves penile length, corrects complex deformities (hourglass, hinge), and provides excellent straightening. Disadvantages include more complex surgery (90-150 minutes), 10-20% risk of new-onset ED from tissue manipulation, potential sensation changes, graft-related complications (rare), and longer recovery. Best for severe curvature preventing intercourse, preserved erectile function worth protecting, adequate length to warrant complex surgery, and patients accepting higher risk for better straightening. Primary Advantages: Preserves/improves length, corrects severe deformities, excellent straightening for complex cases.
For men with both Peyronie's disease and severe erectile dysfunction, implant placement simultaneously addresses both problems. During implant surgery, the device is inflated maximally and manual pressure applied to break up plaques and straighten curvature—called modeling. Additional plication or grafting can be performed if needed. Advantages include solves both ED and curvature with single surgery, reliable erectile function post-operatively, modeling usually sufficient for most curvatures, and cost-effective compared to separate procedures. Best for men with Peyronie's AND severe ED unresponsive to medications—the most definitive single solution. Primary Advantages: Addresses both problems simultaneously, reliable results, cost-effective for dual pathology.
Follow-Up: Wound check at 1-2 weeks; assessment of straightening at 6-8 weeks; sexual activity clearance at 6-8 weeks after complete healing.
Schedule a private, confidential consultation with Dr. Singh in Indore.
Spontaneous resolution of Peyronie’s disease is uncommon but possible, particularly in mild cases during the early acute phase. Studies suggest approximately 5-15% of men experience spontaneous improvement or complete resolution, usually within the first 12-18 months. However, spontaneous improvement is more likely to involve pain resolution rather than significant curvature reduction—the plaque itself rarely disappears completely without treatment. Approximately 40-50% of cases remain stable (no worsening but no improvement), while 30-40% progressively worsen without intervention. Factors favoring spontaneous improvement include early disease (< 6 months), mild curvature (< 30 degrees), minimal plaque formation, and younger age. Given the unpredictable natural history and potential for progression, most urologists recommend at least conservative treatment during the acute phase to maximize chances of stabilization or improvement. The key is early evaluation—waiting months or years to “see what happens” may miss the window for medical interventions that work best during active inflammation phase.
Treatment effectiveness depends heavily on disease stage and severity. For acute phase disease, intralesional collagenase (Xiaflex) injections represent the only FDA-approved therapy with demonstrated efficacy—reducing curvature by approximately 30-40% in clinical trials. However, this requires multiple injection cycles, is expensive, and works best for curvatures 30-90 degrees. Other medical treatments (oral medications, traction, vacuum devices) show limited evidence but may help some patients and are worth trying given low risk. For stable phase disease with significant curvature preventing intercourse, surgical correction is most effective and definitive—penile plication achieves excellent straightening (>90% success) for moderate curvatures with minimal complications, while plaque excision with grafting corrects even severe deformities though with slightly higher complication rates. For men with both Peyronie’s and severe ED, penile implants with modeling are most effective, addressing both problems simultaneously. There’s no single “best” treatment—Dr. Singh individualizes recommendations based on your specific disease characteristics, erectile function status, and personal priorities. The most important factor is treating at the appropriate stage with the appropriate modality.
This is an important expectation to address realistically. Complete restoration to pre-Peyronie’s anatomy is uncommon with any treatment. For non-surgical treatments (medications, injections), even with good response, expect partial improvement—typically 20-40% curvature reduction and minimal to no length restoration. Penile plication surgery effectively straightens curvature (often achieving completely straight or near-straight results) but inherently causes shortening of 1-2 cm because it works by “taking up” the longer side to match the shorter curved side. Plaque excision with grafting can preserve existing length and sometimes restore some lost length by lengthening the shortened side, but rarely achieves full pre-disease length. Penile implants may restore some length lost during flaccid state but erect length remains approximately at the pre-implant Peyronie’s length. Most men lose some length during the natural history of Peyronie’s before treatment even begins due to plaque contracture and tissue remodeling. Realistic expectations are crucial: treatment goals focus on achieving sufficient straightness for vaginal penetration and sexual function (usually <30 degrees residual curvature), minimizing further shortening, and preserving erectile function—rather than perfect cosmetic restoration. Most patients adjust well when properly counseled, prioritizing functional improvement over absolute anatomical perfection.
Surgical correction carries specific risks that require careful consideration. For penile plication, complications include penile shortening (expected, typically 1-2 cm), palpable or visible sutures causing discomfort (5-10%, may require removal), residual or recurrent curvature (5-10%, may need revision), altered sensation (usually temporary), erectile dysfunction (rare <5% as erectile tissue not manipulated), and hematoma or infection (rare). For plaque excision with grafting, risks include new-onset erectile dysfunction (10-20% due to manipulation of erectile tissue), penile shortening despite grafting attempt (still possible), graft-related complications (contraction, poor healing), sensory changes particularly glans numbness (10-20%, often temporary), and all standard surgical risks. For penile implants, risks include infection (1-3%, most serious), mechanical failure (5-10% over 10 years), erosion (<2%), and dissatisfaction with size or rigidity. All surgeries carry risks of bleeding, pain, scarring, and anesthesia complications. Dr. Singh’s extensive surgical experience minimizes these risks substantially. Importantly, no surgery comes with 100% guarantee of perfect results—residual curvature <30 degrees is often acceptable as it doesn’t prevent intercourse. Despite these risks, patient satisfaction rates exceed 70-80% for appropriate surgical candidates because functional improvement significantly outweighs risks for men whose Peyronie’s prevents satisfying sexual activity.
Recovery timelines vary by treatment modality. For injection therapy (collagenase, verapamil), there’s minimal recovery—injections cause temporary swelling and discomfort for 24-48 hours, but normal activities can continue. Sexual activity should be avoided for 2-3 days after each injection. Multiple injection cycles occur over weeks to months. For surgical procedures, recovery is more substantial. Hospital stay is typically outpatient to overnight. Pain is moderate, managed with oral medications for 5-7 days. Swelling and bruising peak at 3-5 days and gradually resolve over 2-3 weeks. Dressings are removed after 48-72 hours. Sutures are absorbable (no removal needed). Light activities can resume within 1 week, return to desk work in 7-10 days, and full non-strenuous activities by 3-4 weeks. Sexual activity must be avoided for 6-8 weeks to allow complete wound healing and tissue maturation—premature activity risks wound dehiscence, bleeding, curvature recurrence, or implant complications. After clearance at 6-8 weeks, sexual activity should be resumed gradually. Initial attempts may feel different due to altered anatomy or psychological adjustment. Most men report comfortable, satisfying intercourse by 8-12 weeks post-surgery. Patience during recovery is essential for optimal outcomes.
Yes, Peyronie’s disease and erectile dysfunction (ED) are intimately connected. Studies show 40-55% of men with Peyronie’s also have ED, which may result from multiple factors: mechanical inability to achieve full rigidity due to inelastic plaque preventing expansion, vascular changes (plaques can compress penile arteries reducing blood flow), psychological factors (anxiety, depression, embarrassment about curvature), and coexisting risk factors (diabetes, cardiovascular disease, aging affecting both conditions). The relationship is bidirectional—curvature makes intercourse mechanically difficult even with adequate erection, while ED makes curvature assessment and treatment more complex. Treatment approach depends on which problem predominates. If erectile function is reasonable but curvature prevents intercourse, curvature-focused treatments (injections, plication, grafting) are appropriate. If significant ED coexists, treating ED first with medications (PDE5 inhibitors like Viagra) may improve both erection quality and apparent curvature severity. If severe ED doesn’t respond to medications and significant curvature exists, penile implant with modeling addresses both problems definitively in one surgery—often the most practical solution for dual pathology. Dr. Singh thoroughly evaluates both erectile function and curvature during consultation, using pharmacologic erection testing when needed, to determine whether ED is primary, secondary to Peyronie’s, or an independent coexisting problem requiring its own management.
24/7 Services Available
Copyright © 2026 Urology Center | All Rights Reserved
Design and Developed by Namastetu Technologies Pvt.Ltd