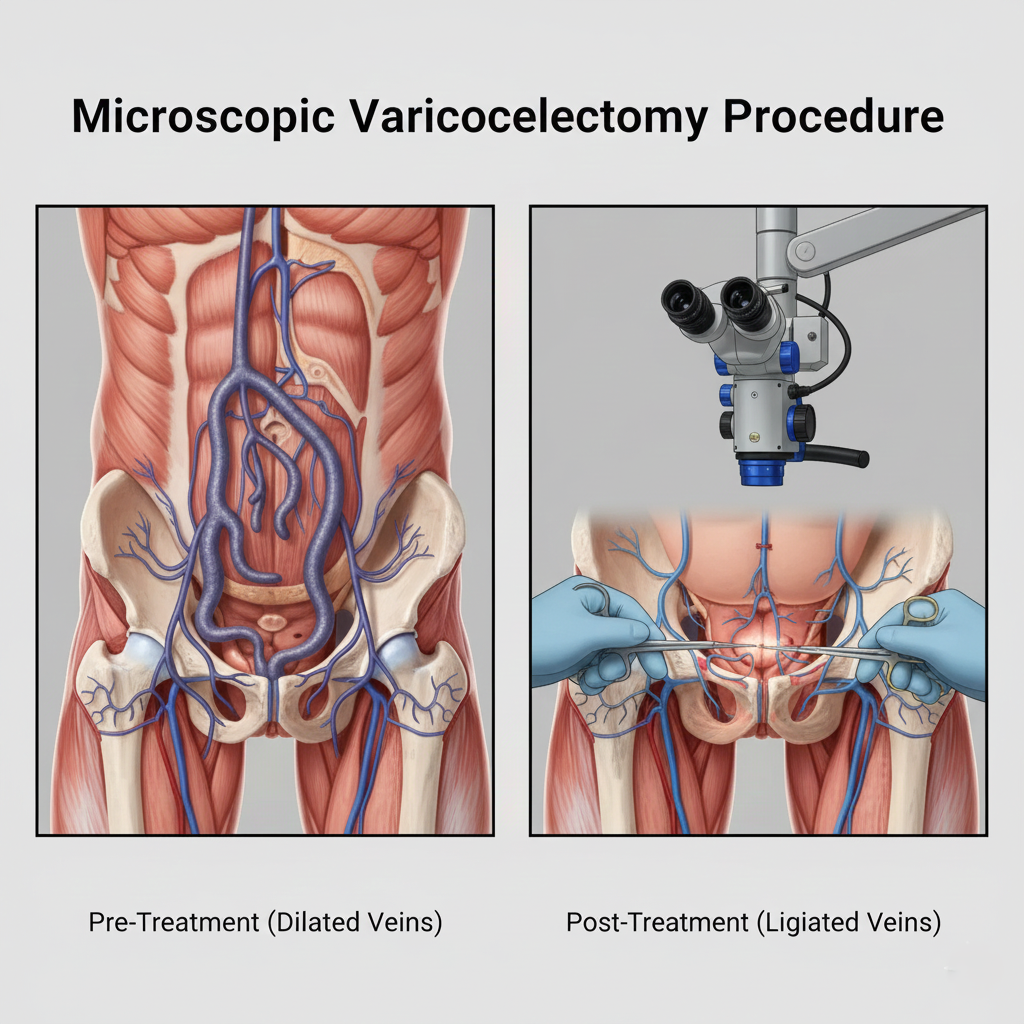
Dr. Vikas Singh is a highly skilled Consultant Urologist and Andrologist in Indore, specializing in advanced surgical treatment for Varicocele—the most common correctable cause of male infertility. With extensive training in microsurgical techniques and andrology, he performs Microscopic Varicocelectomy using operating microscope magnification for superior precision, minimal complications, and optimal fertility outcomes. This gold-standard technique offers significantly better results than conventional open or laparoscopic approaches, with success rates exceeding 90% in improving sperm parameters and lower complication rates (hydrocele formation <1% vs. 10-15% with non-microscopic methods). Practicing at Kokilaben Dhirubhai Ambani Hospital Indore with access to specialized microsurgical equipment, advanced sperm analysis facilities, and comprehensive fertility services, Dr. Singh provides the complete spectrum of care from diagnosis through post-operative fertility monitoring. His approach emphasizes achieving both symptomatic relief and fertility improvement while minimizing risks to testicular function and future reproductive potential. We maintain complete transparency regarding treatment costs and provide comprehensive insurance assistance for our patients across Central India.
Consultant Surgeon at Kokilaben Dhirubhai Ambani Hospital, Indore, with specialized microsurgical capabilities and andrology laboratory.
Advanced fellowship in microsurgical techniques including varicocelectomy, vasectomy reversal, and testicular procedures.
Exceptional outcomes in improving sperm parameters and achieving pregnancies with minimal complication rates.
Varicocele is an abnormal enlargement of the pampiniform plexus—the network of veins draining the testicle—similar to varicose veins in the legs. These dilated veins cause pooling of blood around the testicle, raising scrotal temperature and disrupting normal testicular function. Varicoceles occur in 15-20% of all men but affect 35-40% of men with primary infertility and 70-80% of men with secondary infertility (unable to conceive after previously fathering children). They're more common on the left side (85-90%) due to anatomical factors.
Varicoceles impair fertility through multiple mechanisms: elevated testicular temperature (even 1-2°C increase damages sperm production), oxidative stress (increased free radicals damaging sperm DNA), hormonal imbalances (reduced testosterone, impaired Leydig cell function), hypoxia (reduced oxygen delivery to testicular tissue), and reflux of toxic metabolites from kidney and adrenal veins. These factors result in abnormal semen parameters—reduced sperm count (oligospermia), poor motility (asthenospermia), abnormal morphology (teratospermia), and DNA fragmentation—all reducing natural conception chances and potentially affecting assisted reproduction success rates.
While many varicoceles are asymptomatic and discovered during infertility workup, symptomatic varicoceles can cause dull, aching scrotal pain (worse after prolonged standing, exercise, or end of day), visible or palpable scrotal swelling ("bag of worms" feel), testicular atrophy (smaller affected testicle), and sensation of heaviness or dragging in scrotum. Pain severity doesn't correlate with fertility impact—large, symptomatic varicoceles and small, asymptomatic ones can both significantly affect sperm quality.
Diagnosis begins with thorough scrotal examination in standing position with and without Valsalva maneuver (bearing down increases pressure, making varicoceles more prominent). Varicoceles are graded: Grade I (palpable only with Valsalva), Grade II (palpable without Valsalva), Grade III (visible through scrotal skin). Testicular volume is measured with orchidometer to detect atrophy. While physical examination is primary diagnostic tool, it’s supplemented with additional studies.
Color Doppler ultrasound provides objective confirmation, measuring vein diameter (>3mm indicates varicocele), documenting reflux pattern with Valsalva, assessing testicular size and texture, and ruling out other pathology (tumors, hydroceles). Ultrasound is particularly valuable for subclinical varicoceles (not palpable but detectable on imaging), assessing bilateral involvement, and providing baseline for post-operative comparison.
Multiple semen analyses (2-3 specimens, 2-4 weeks apart) establish baseline fertility parameters including sperm concentration, motility, morphology, volume, and pH. Advanced testing may include sperm DNA fragmentation, oxidative stress markers, and hormonal evaluation (testosterone, FSH, LH). This documentation is crucial for treatment decision-making and measuring post-operative improvement. Even men with normal semen parameters may benefit from repair if varicocele is causing pain or progressive testicular atrophy.
The operating microscope (15-25x magnification) allows precise identification and preservation of the testicular artery, lymphatic vessels, and vas deferens while selectively ligating all dilated veins. This precision dramatically reduces complications: hydrocele formation <1% (vs. 10-15% with non-microscopic techniques), testicular atrophy virtually eliminated (vs. 1-3% with ligation of arteries), and varicocele recurrence <1% (vs. 5-15% with inadequate vein ligation). The microscopic approach also allows identification of tiny collateral veins often missed with naked eye or loupes, ensuring complete varicocele elimination.
Surgery is performed under general or spinal anesthesia. A small inguinal incision (2-3 cm) is made at the level of the external inguinal ring—above the scrotum but below the abdomen. The spermatic cord is identified and delivered into the wound. Using the operating microscope, Dr. Singh meticulously identifies and preserves 1-3 testicular arteries (critical for testicular blood supply), multiple lymphatic channels (preventing hydrocele), the vas deferens (sperm transport), and cremasteric vessels and nerves. All internal spermatic veins (typically 5-15 veins of varying sizes) are identified, isolated, ligated with fine sutures, and divided. External spermatic and gubernacular veins are also ligated. The entire dissection takes 60-90 minutes per side.
The incision is closed with absorbable sutures. A scrotal support and ice packs minimize swelling. Hospital stay is typically day surgery or overnight. Pain is mild to moderate, managed with oral medications. Patients go home the same day or the next morning with detailed instructions for optimal recovery and minimal complications.
This approach offers optimal outcomes through high magnification allowing preservation of arteries and lymphatics, access to all venous collaterals at inguinal level, lowest complication rates (hydrocele <1%, recurrence <1%, artery injury virtually zero), highest fertility improvement rates (70-80% show semen improvement, 40-50% achieve pregnancies), and reasonable recovery (return to work 3-5 days, full activities 2-3 weeks). Disadvantages include longer operative time (requires microscope skills), higher cost due to specialized equipment, and requires surgeon training in microsurgery. Best for all patients seeking optimal fertility outcomes with minimal risk.
Primary Advantages: Lowest complications, highest success, best preservation of testicular function.
Traditional approach using naked eye or loupes (2-4x magnification) to ligate veins at inguinal or higher level. Faster procedure but significantly higher complication rates: hydrocele 10-15% (from lymphatic injury), arterial injury 1-3% (causing testicular atrophy), recurrence 5-15% (missing small veins), and lower fertility improvement. Largely abandoned at specialized centers in favor of microscopic technique.
Key Limitations: High complication rates, suboptimal outcomes, superseded by microscopic approach.
Uses laparoscopic instruments to ligate veins in the high abdomen. Advantages include small incisions and potentially faster recovery. Disadvantages include the inability to preserve lymphatics or the testicular artery (both too small to see at this level), higher hydrocele rates (7-10%), higher recurrence (collateral veins missed), requires general anesthesia, and risk of intra-abdominal complications. May be considered for bilateral varicoceles or in specific situations, but generally inferior to microscopic inguinal approach for fertility outcomes. Key Limitations: Cannot preserve critical structures, higher complications than microscopic technique.
70-80% of men show improved sperm parameters post-operatively; 40-50% achieve natural pregnancies within 12-18 months.
Hydrocele <1%, recurrence <1%, arterial injury virtually zero—dramatically lower than all other techniques.
Microscopic preservation of arteries maintains optimal testicular blood supply, hormone production, and long-term function.
Over 90% of men with scrotal pain experience significant improvement or complete resolution after surgery.
Schedule a private, confidential consultation with Dr. Singh in Indore.
Microscopic varicocelectomy has excellent success rates for both semen parameter improvement and pregnancy achievement. Meta-analyses show approximately 70-80% of men experience significant improvement in at least one semen parameter (count, motility, or morphology) after surgery. The degree of improvement varies—some men see dramatic increases (oligospermic becoming normospermic), while others show modest improvements that may still meaningfully impact fertility. Regarding pregnancies, studies demonstrate 40-50% of couples achieve natural conception within 12-18 months post-surgery who were previously infertile. Factors predicting better outcomes include younger age (men <35 have better improvement), larger varicocele grade (Grade II-III benefit more than Grade I), pre-operative sperm count >5 million/ml (men with very low counts may still need assisted reproduction), and shorter duration of infertility (<3 years better than >5 years). Even men who don’t achieve natural pregnancy often have improved sperm parameters that enhance success rates of IUI or IVF if needed. Importantly, varicocelectomy also may prevent progressive deterioration in men with declining sperm counts over time, preserving future fertility potential.
The fundamental difference is surgical precision through magnification and approach. Microscopic varicocelectomy uses an operating microscope providing 15-25x magnification, allowing the surgeon to identify and individually isolate tiny structures: 1-3 testicular arteries (0.5-1mm diameter) providing critical blood supply, 8-12 lymphatic channels (even smaller) whose preservation prevents hydrocele formation, and all 5-15 internal spermatic veins of varying sizes for complete varicocele elimination. This precision results in complication rates under 1-2%. Conventional “regular” varicocelectomy uses naked eye or surgical loupes (2-4x magnification), making arteries and lymphatics difficult or impossible to identify individually—they’re often ligated en masse with veins. This causes hydrocele in 10-15% of cases (from lymphatic damage) and testicular atrophy in 1-3% (from arterial injury). Recurrence rates are also higher (5-15% vs. <1%) because small collateral veins are missed without high magnification. From a patient perspective, microscopic technique requires a fellowship-trained microsurgeon and longer operative time but delivers dramatically superior outcomes. The choice is clear for men prioritizing fertility outcomes and minimal complications—microscopic is the gold standard at specialized centers.
This is an important emerging benefit of varicocelectomy beyond fertility. Recent studies demonstrate that varicocele repair can significantly improve testosterone levels in men with hypogonadism (low testosterone). Research shows approximately 70-80% of hypogonadal men (testosterone <300 ng/dL) experience meaningful increases in testosterone post-varicocelectomy—average increases of 100-150 ng/dL, often sufficient to bring levels into normal range without needing testosterone replacement therapy. The mechanism involves restoring normal testicular temperature and function, improving Leydig cell performance (cells producing testosterone), and reducing oxidative stress that impairs hormone synthesis. This benefit occurs in addition to improved sperm production, making varicocelectomy particularly valuable for men with both infertility and hypogonadism symptoms (low libido, erectile dysfunction, fatigue, decreased muscle mass). Importantly, varicocele repair preserves natural testosterone production and fertility potential, whereas testosterone replacement therapy actually suppresses sperm production—making surgery the preferred approach for men wanting both improved testosterone AND maintained fertility. Dr. Singh measures baseline testosterone levels during infertility workup and monitors post-operative improvement as part of comprehensive andrology care.
Microscopic varicocelectomy is very safe, but no surgery is completely risk-free. Complication rates are remarkably low with microscopic technique but should be understood. Minor complications include wound infection (<1%, treated with antibiotics), hematoma or bleeding (1-2%, usually resolves spontaneously or with drainage), temporary scrotal swelling or bruising (common, resolves in 1-2 weeks), and incisional pain persisting beyond expected timeframe (rare, usually resolves with time). Technique-specific complications that microscopy minimizes include hydrocele formation (<1% with microscopic vs. 10-15% non-microscopic—caused by lymphatic injury, may require secondary drainage procedure), testicular atrophy (<0.5% with microscopic vs. 1-3% non-microscopic—from arterial injury causing testicular damage), and varicocele recurrence or persistence (<1-2% with microscopic vs. 5-15% non-microscopic—from missed collateral veins). Extremely rare complications include injury to vas deferens, nerve damage causing groin numbness, or chronic pain syndrome. General surgical risks include anesthesia complications and thromboembolic events (very rare). Dr. Singh’s microsurgical expertise and meticulous technique minimize all these risks substantially. The benefit-to-risk ratio strongly favors surgery for appropriate candidates—the potential for fertility improvement and symptom relief far outweighs minimal complication risks.
Sperm improvement follows a predictable but somewhat prolonged timeline because spermatogenesis (sperm production) takes approximately 72-90 days. The varicocelectomy creates improved testicular environment immediately, but sperm currently in production were already affected by the varicocele. Here’s the typical timeline: Months 0-3 post-surgery involve healing and early testicular recovery—sperm parameters may initially remain unchanged or even temporarily worsen due to surgical inflammation. Month 3 is when first post-operative semen analysis is performed—early improvements may be visible but optimal benefit hasn’t occurred yet. Months 3-6 see progressive improvement as new sperm produced in improved environment mature and appear in ejaculate. Month 6 is when second semen analysis definitively documents improvement—maximum benefit is typically achieved by this point. Months 6-18 represent optimal conception window—couples should actively attempt pregnancy during this period when sperm quality is best. Dr. Singh recommends beginning conception attempts around month 3-4 (no need to wait for perfect sperm parameters) but expectations should be realistic that peak fertility occurs 6-12 months post-surgery. If pregnancy doesn’t occur by 12-18 months despite good sperm improvement, consideration for assisted reproductive technologies (IUI, IVF) may be appropriate. Importantly, even men who require assisted reproduction benefit from varicocelectomy as improved sperm quality enhances success rates of these technologies.
Recurrence or persistence of varicocele after surgery can occur but is rare with proper microscopic technique—less than 1-2% compared to 5-15% with non-microscopic methods. Recurrence happens when collateral venous pathways that were too small to identify at initial surgery enlarge over time, or when skip lesions (venous segments that weren’t dilated initially) later become varicose. Persistence occurs when some veins are missed during initial surgery. The microscopic approach dramatically reduces this risk because high magnification allows identification of all venous branches and collaterals that non-microscopic surgeons miss. If recurrence occurs, symptoms include return of scrotal swelling, recurrence of pain if that was initial complaint, or re-deterioration of semen parameters after initial improvement. Diagnosis is confirmed with physical examination and Doppler ultrasound. Treatment options include observation if recurrence is small and asymptomatic with stable semen parameters, repeat microsurgical varicocelectomy (success rates for redo surgery are good, 80-85%), or consideration for radiologic embolization (catheter-based vein occlusion). Fortunately, with Dr. Singh’s microsurgical expertise, true recurrence requiring re-intervention is exceptionally rare. Regular follow-up with semen analysis and occasional physical examinations allow early detection if recurrence occurs.
24/7 Services Available
Copyright © 2026 Urology Center | All Rights Reserved
Design and Developed by Namastetu Technologies Pvt.Ltd