Dr. Vikas Singh is a distinguished Consultant Urological Oncologist in Indore, specializing in advanced kidney-sparing surgery for renal tumors. With extensive expertise in both Laparoscopic and Robotic Partial Nephrectomy, he offers patients with small to moderate kidney tumors the opportunity to preserve healthy kidney tissue while achieving complete cancer removal. This nephron-sparing approach is the modern gold standard for localized renal masses, providing equivalent cancer control to radical nephrectomy (complete kidney removal) while significantly preserving long-term renal function and reducing risks of chronic kidney disease, cardiovascular complications, and the need for dialysis. Practicing at Kokilaben Dhirubhai Ambani Hospital Indore with access to the Da Vinci Robotic System and advanced laparoscopic equipment, Dr. Singh achieves optimal oncologic outcomes with minimal invasiveness, faster recovery, and superior preservation of kidney function. His comprehensive approach emphasizes accurate tumor staging, precise surgical technique minimizing warm ischemia time, and thorough post-operative monitoring to ensure both cancer cure and kidney health. We maintain complete transparency regarding treatment costs and provide comprehensive insurance assistance for our patients across Central India.
Consultant Surgeon at Kokilaben Dhirubhai Ambani Hospital, Indore, equipped with Da Vinci Robotic System for advanced procedures.
Extensive expertise in urological oncology with hundreds of successful partial nephrectomies performed.
Specialized techniques minimizing warm ischemia time and maximizing preservation of healthy kidney tissue.
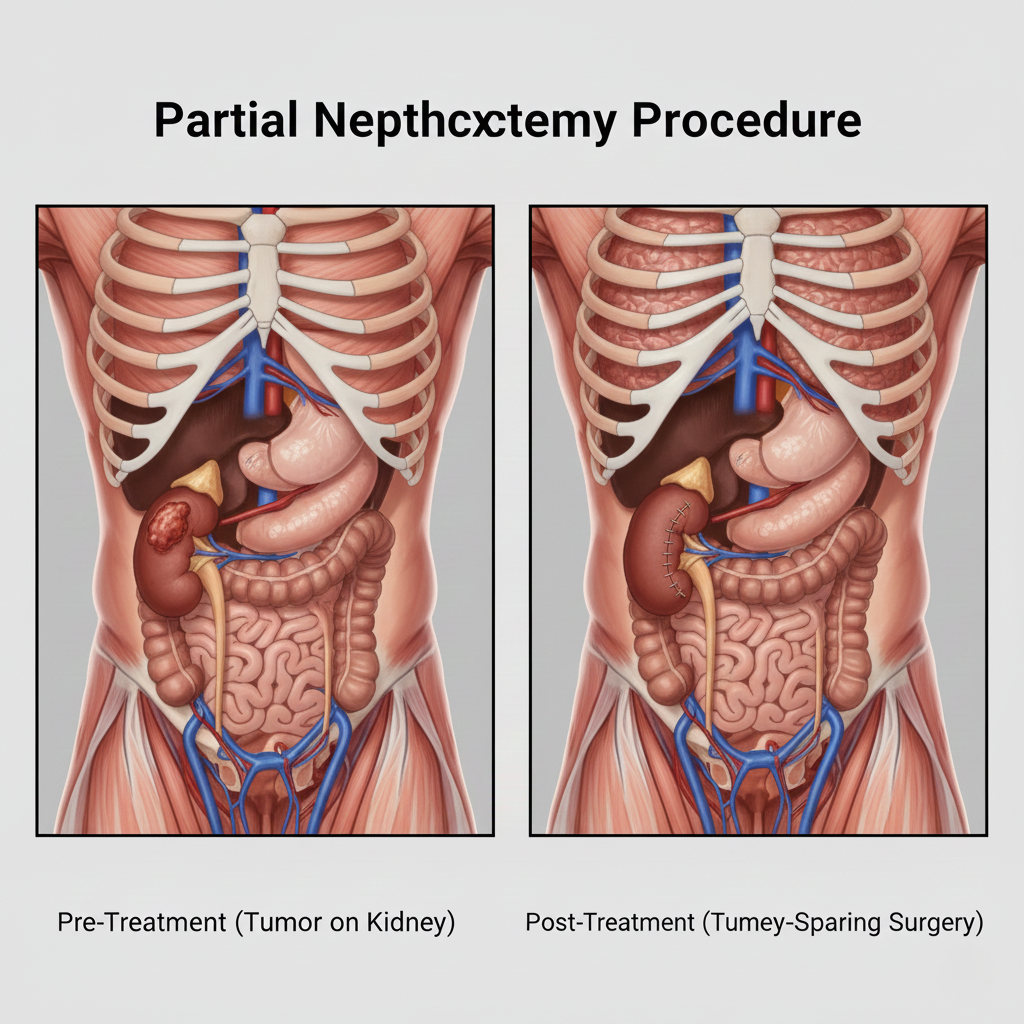
Partial Nephrectomy (also called nephron-sparing surgery) involves surgically removing only the tumor and a small margin of surrounding healthy tissue while preserving the remainder of the kidney. This contrasts with radical nephrectomy where the entire kidney is removed. Modern imaging and surgical techniques allow safe partial nephrectomy for tumors up to 7 cm and sometimes larger, depending on location. The procedure aims to achieve two critical goals simultaneously: complete cancer removal with negative surgical margins (trifecta: negative margins, preserved renal function, no complications) and maximum preservation of healthy kidney parenchyma.
Preserving kidney function has profound long-term health implications beyond cancer treatment. Studies demonstrate that patients maintaining bilateral kidney function (even if one kidney is partially removed) have significantly lower risk of chronic kidney disease progression, reduced cardiovascular morbidity and mortality, lower risk of requiring dialysis, better quality of life, and improved overall survival compared to those with single kidney after radical nephrectomy. Even small amounts of preserved kidney tissue provide measurable health benefits. This is particularly important for younger patients, those with diabetes or hypertension, patients with solitary kidney, and individuals with hereditary kidney cancer syndromes requiring future surgeries.
Partial nephrectomy is now the standard of care for T1a tumors (<4 cm) and strongly recommended for T1b tumors (4-7 cm) when technically feasible. It's also indicated for imperative situations: solitary kidney (only one functioning kidney), bilateral kidney tumors, hereditary renal cancer syndromes (Von Hippel-Lindau, hereditary papillary RCC), and pre-existing chronic kidney disease where preserving function is critical. Even for patients with two normal kidneys and favorable anatomy for radical nephrectomy, partial nephrectomy is preferred due to superior long-term outcomes.
The Da Vinci Robotic System offers the most advanced platform for partial nephrectomy, providing 10x magnified 3D high-definition visualization, wristed instruments with seven degrees of motion mimicking human wrist (enabling precise tumor excision and complex reconstructive suturing), tremor filtration and motion scaling for microsurgical precision, and ergonomic console allowing surgeon optimal control during demanding procedures. These features translate to superior outcomes: more precise tumor excision with minimal normal tissue removal, faster, more precise renorrhaphy (kidney reconstruction) reducing warm ischemia time, lower conversion to radical nephrectomy rates, and potentially lower complication rates. Best for complex tumors (central, hilar, endophytic), challenging locations requiring intricate dissection, and patients prioritizing maximum kidney preservation with cutting-edge technology. Primary Advantages: Ultimate precision, minimal tissue loss, optimal for complex tumors, shorter warm ischemia time.
Pure laparoscopic approach uses traditional laparoscopic instruments without robotic assistance. Requires high degree of laparoscopic suturing expertise for kidney reconstruction. Advantages include minimally invasive with small incisions, shorter hospital stay than open surgery, lower cost than robotic approach (no robot fees), and excellent outcomes in experienced hands for favorable anatomy tumors. Disadvantages include more technically challenging than robotic (particularly reconstruction phase), longer learning curve for surgeons, potentially longer warm ischemia time for complex cases, and more difficult for centrally located or deeply embedded tumors. Best for peripheral, exophytic tumors in patients where robotic system isn’t available or cost is prohibitive. Primary Advantages: Minimally invasive, proven outcomes, lower cost than robotic, no robot dependency.
Traditional surgery through flank incision, rarely performed now except for very large/complex tumors or situations where minimally invasive approach isn’t feasible. Allows direct tactile feedback and may be necessary for T2 tumors (>7 cm) or extensive vascular involvement. Recovery is longer with more post-operative pain and 5-7 day hospital stay. Modern practice reserves open approach for specific clinical scenarios where minimally invasive techniques would compromise oncologic or functional outcomes.
High-resolution CT or MRI with contrast defines tumor size, location, depth, relationship to collecting system and blood vessels, and renal anatomy. Nephrometry scoring systems (R.E.N.A.L. score) assess tumor complexity helping predict surgical difficulty and outcomes. Dr. Singh reviews imaging meticulously, planning surgical approach, identifying vessels requiring clamping, and determining reconstruction strategy. Pre-operative optimization includes cardiovascular assessment, kidney function baseline (eGFR, creatinine), and medical management of comorbidities.
Under general anesthesia, robotic or laparoscopic ports are placed. The kidney is mobilized and the tumor identified. Renal hilum (artery and vein) is carefully dissected and prepared for clamping. Selective clamping (only the vessels supplying tumor-containing segment) is preferred over global clamping when anatomy permits, minimizing ischemia to healthy kidney tissue. Once blood flow is stopped (warm ischemia begins), the tumor is precisely excised with surrounding margin (typically 5-10mm). The resection bed is inspected for bleeding and collecting system entry (repaired if present). The kidney is reconstructed with meticulous multi-layer suturing—inner layer closes collecting system, middle layer approximates parenchyma, outer layer reinforces with bolsters. Clamps are released (reperfusion) and hemostasis confirmed. Goal is warm ischemia time <25 minutes, ideally <20 minutes, to minimize kidney damage.
Patients are monitored in recovery, then transferred to ward. A surgical drain is typically placed temporarily. Hospital stay is 2-4 days for robotic/laparoscopic approach. Kidney function is monitored closely (serum creatinine) to assess preserved function. Pathology confirms tumor type, grade, and negative margins. Follow-up protocol includes regular imaging and kidney function tests to monitor for recurrence and renal health.
Maintains maximum healthy kidney tissue, protecting against chronic kidney disease, cardiovascular disease, and dialysis risk long-term.
Provides same excellent oncologic outcomes as radical nephrectomy for appropriately selected tumors—five-year cancer-specific survival >95% for T1 tumors.
Small incisions result in less pain, shorter hospital stay (2-4 days vs. 5-7 for open), faster recovery, and quicker return to activities.
Patients maintain better overall health, reduced medical complications, and improved long-term survival compared to radical nephrectomy.
Schedule a private, confidential consultation with Dr. Singh in Indore.
Most patients with small renal masses (T1a <4cm, T1b 4-7cm) are excellent candidates for partial nephrectomy. Critical factors include tumor size and location (peripheral tumors easier than central/hilar), kidney function (patients with compromised function benefit most from preservation), solitary kidney status (partial mandatory if only one kidney), and overall health. Modern techniques allow partial nephrectomy even for complex tumors previously requiring radical removal. Dr. Singh evaluates detailed imaging, assesses nephrometry scores, and discusses individualized recommendations. Unless the tumor is extremely large, deeply invasive, or involves critical structures making safe preservation impossible, partial nephrectomy is typically preferred.
Warm ischemia time is the duration renal blood vessels are clamped during tumor removal, temporarily cutting off blood supply to the kidney. During this period, the kidney receives no oxygen (ischemia), potentially causing tissue damage. Each minute of warm ischemia causes progressive injury—prolonged ischemia reduces post-operative kidney function. Studies show warm ischemia <25 minutes is generally safe, with optimal target <20 minutes. Robotic surgery’s enhanced visualization and dexterity allows faster, more precise reconstruction, minimizing ischemia time. Dr. Singh’s expertise and meticulous technique consistently achieve optimal warm ischemia times, maximizing kidney function preservation.
Partial nephrectomy provides equivalent cancer control to radical nephrectomy for T1 tumors. Multiple large studies show identical cancer-specific survival rates (>95% at 5 years for T1a, >90% for T1b) between partial and radical approaches when appropriate surgical margins are achieved. The key is negative surgical margins—removing tumor completely with surrounding healthy tissue rim. Modern imaging and surgical techniques ensure accurate tumor excision. While local recurrence rates are slightly higher with partial nephrectomy (2-5% vs. <1%), these recurrences are typically detected early through surveillance and successfully treated. The survival benefit from preserved kidney function outweighs minimal recurrence risk differences.
Partial nephrectomy is generally safe but more technically complex than radical nephrectomy, carrying specific risks. Complications include bleeding requiring transfusion (5-10%, higher in complex cases) or rarely reoperation, urine leak from collecting system injury (2-5%, usually resolves with prolonged drain or stent placement), loss of remaining kidney function requiring conversion to radical nephrectomy during surgery (2-5% for complex tumors), acute kidney injury from prolonged warm ischemia (usually recovers with supportive care), pseudoaneurysm or arteriovenous fistula (rare <2%, may require embolization), and infection or wound complications (1-3%). Dr. Singh’s extensive experience minimizes these risks through meticulous technique and careful patient selection.
Most patients maintain excellent kidney function after partial nephrectomy. The amount of function preserved depends on how much healthy tissue remains, warm ischemia time (shorter is better), baseline kidney function before surgery, and post-operative recovery. On average, patients lose 10-20% of total kidney function (both kidneys combined) after partial nephrectomy—far less than the 40-50% loss with radical nephrectomy. For example, if your preoperative eGFR was 80, it might decrease to 65-70 post-operatively—still excellent function. Need for dialysis after partial nephrectomy is extremely rare (<1%) unless patient had severely compromised baseline function or major complications. Long-term kidney health remains stable or slowly declines with aging as it would normally.
Recovery timeline varies by surgical approach and individual factors. Light walking is encouraged immediately. Driving can resume when off narcotic pain medications and comfortable (typically 1-2 weeks). Desk work typically resumes 2-3 weeks post-surgery once energy levels recover. Strenuous exercise, heavy lifting (>10 pounds), and physically demanding work should be avoided for 6-8 weeks to allow complete internal healing and prevent complications like bleeding or hernia. Sexual activity can typically resume 4-6 weeks after surgery once comfortable. Dr. Singh provides personalized return-to-activity guidance based on your specific procedure complexity, recovery progress, and occupation demands during follow-up visits.
24/7 Services Available
Copyright © 2026 Urology Center | All Rights Reserved
Design and Developed by Namastetu Technologies Pvt.Ltd